Our children are fatter now than in many decades and if we allow this to continue as parents and teachers and coaches and mentors, we allow them to grow into diseased adults. If you don’t believe me, the statistics from the Centers for Disease Control (CDC) are scary:
“The percentage of children with obesity in the United States has more than tripled since the 1970s. Today, about one in five school-aged children (ages 6–19) has obesity.”
Most children do not feed themselves and their brains are not mature enough to make good decisions about food and physical activity. It is we adults who need to step in and prevent our future generation of adults and leaders from being disease bound and living in poor quality of life. Some recent studies shed light on some of the strongest ways forward.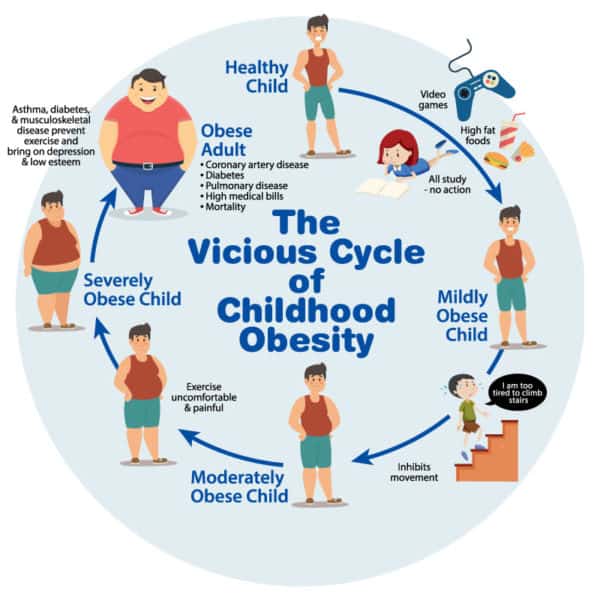
Negative Broader Effects of Childhood Obesity
Before we look at solutions provided by a few studies, I wanted to share additional statistics on childhood obesity. I have a son in college and three girls in elementary/middle school, and see more overweight and obese children in the primary schools today than even when my son was there. Yet, when I talk to parents, they seem oblivious because “everyone is beautiful the way they are.” That is true for self-esteem and perhaps spiritual growth, but not when it comes to health and disease prevention. Let’s take a look at what the CDC has to say about the immediate and long-term impacts of childhood obesity on physical, social, and emotional health.
-
Children with obesity are at higher risk for having other chronic health conditions and diseases that impact physical health, such as asthma, sleep apnea, bone and joint problems, type 2 diabetes, and risk factors for heart disease.
-
Children with obesity are bullied and teased more than their normal weight peers, and are more likely to suffer from social isolation, depression, and lower self-esteem.
-
In the long term, childhood obesity also is associated with having obesity as an adult, which is linked to serious conditions and diseases such as heart disease, type 2 diabetes, metabolic syndrome, and several types of cancer.
Those statements are cries for help. Let’s now look toward solutions.
Obese Kids Do Best with Intensive Lifestyle-based Interventions
According to the conclusions of the US Preventive Service Task Force, based on 42 lifestyle-based intervention trials, more than 26 hours of direct-contact behavioral interventions results in improved weight status; and these results can last up to a year. Therefore, they recommend that clinicians screen for obesity in children ages six to 19 and provide or refer them to comprehensive, intensive behavioral [lifestyle based] intervention programs for weight loss.
The Task Force followed up by clarifying the truly multi-disciplinary approach that is needed, including:
- Individual counseling sessions
- Combined parent and child sessions
- Dietary counseling Self-monitoring coaching, and
- Supervised physical activity sessions.
Community Intervention Provides Success
Community intervention was shown elsewhere to provide modest results in weight loss among obese children, in a relatively short period of time.
According to reporting by MedPage Today, among seventh graders in one community study the prevalence of obesity dropped by over 2% compared with the control group at baseline. What’s more, fourth and seventh graders reported consuming less sugar-sweetened beverages and more water while also reducing their TV and computer gaming times.
According to the researchers in the story, “These findings add important empirical evidence to the body of literature concerning multilevel, multi-sector, community-based interventions and may inform the design of future obesity prevention efforts.” What’s more, they assert that engagement across levels and setting is critical for overcoming obesity and its risks. 
Conclusion
There are many causes of the obesity epidemic, especially among the youth of our country. The fast rise of technology for games and leisure, and their use is non-local communication, leads kids to be more sedentary, more solitary and less active. Add to this low quality of food in our children’s school, the amount of toxic chemicals in foods that affect genes and organ function, and the proliferation of low-quality, low-nutritious, simple carbohydrate foods and snacks, and the issue becomes clear.
To overcome this problem, the Committee on Accelerating Progress in Obesity Prevention has outlined the following “five key recommendations to accelerate meaningful change on a societal level during the next decade”:
- 1) Major reforms in access to and opportunities for physical activity;
- 2) Widespread reductions in the availability of unhealthy foods and beverages and increases in access to healthier options at affordable, competitive prices;
- 3) An overhaul of the messages that surround Americans through marketing and education with respect to physical activity and food consumption;
- 4) Expansion of the obesity prevention support structure provided by health care providers, insurers, and employers; and
- 5) Schools as a major national focal point for obesity prevention.

